Replacement Parts - comfort zone fan replacement parts
Wilson SR. The gastrointestinal tract. In: Rumack CM, Levine D, eds. Diagnostic Ultrasound. 5th ed. Philadelphia, PA: Elsevier; 2018:chap 8.
Hypoxia-induced pulmonary hypertension (PH) is one of the most common and deadliest forms of PH. Fibroblast growth factor receptors 1 and 2 (FGFR1/2) are elevated in patients with PH and in mice exposed to chronic hypoxia. Endothelial FGFR1/2 signaling is important for the adaptive response to several injury types and we hypothesized that endothelial FGFR1/2 signaling would protect against hypoxia-induced PH. Mice lacking endothelial FGFR1/2, mice with activated endothelial FGFR signaling, and human pulmonary artery endothelial cells (HPAECs) were challenged with hypoxia. We assessed the effect of FGFR activation and inhibition on right ventricular pressure, vascular remodeling, and endothelial-mesenchymal transition (EndMT), a known pathologic change seen in patients with PH. Hypoxia-exposed mice lacking endothelial FGFRs developed increased PH, while mice overexpressing a constitutively active FGFR in endothelial cells did not develop PH. Mechanistically, lack of endothelial FGFRs or inhibition of FGFRs in HPAECs led to increased TGF-β signaling and increased EndMT in response to hypoxia. These phenotypes were reversed in mice with activated endothelial FGFR signaling, suggesting that FGFR signaling inhibits TGF-β pathway–mediated EndMT during chronic hypoxia. Consistent with these observations, lung tissue from patients with PH showed activation of FGFR and TGF-β signaling. Collectively, these data suggest that activation of endothelial FGFR signaling could be therapeutic for hypoxia-induced PH.
Nickels LC, Duran-Gehring P. Emergency ultrasound. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap e3.
Barnett CF, Sweeney DA, Huddleston LL. Ultrasonography: advanced applications and procedures. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 24.Chen L. Abdominal ultrasound imaging: anatomy, physics, instrumentation, and technique. In: Sahani DV, Samir AE, eds. Abdominal Imaging. 2nd ed. Philadelphia, PA: Elsevier; 2017:chap 3.Levine MS, Gore RM. Diagnostic imaging procedures in gastroenterology. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 124.Nickels LC, Duran-Gehring P. Emergency ultrasound. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap e3.Wilson SR. The gastrointestinal tract. In: Rumack CM, Levine D, eds. Diagnostic Ultrasound. 5th ed. Philadelphia, PA: Elsevier; 2018:chap 8.
Levine MS, Gore RM. Diagnostic imaging procedures in gastroenterology. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 124.
Abdominal ultrasound is a scanning technique used to image the interior of the abdomen. Like the X-ray, MRI, and CT scan, it has its place as a diagnostic tool. Ultrasound scans use high frequency sound waves to produce an image and do not expose the individual to radiation. The procedure is painless and safe.
You may have this test to: Find the cause of abdominal painFind the cause of kidney infectionsDiagnose or monitor tumors and cancersDiagnose or treat ascitesLearn why there is swelling of an abdominal organLook for damage after an injuryLook for stones in the gallbladder or kidneyLook for the cause of abnormal blood tests such as liver function tests or kidney testsLook for the cause of a fever The reason for the test will depend on your symptoms.
The kidneys are responsible for removing wastes from the body, regulating electrolyte balance and blood pressure, and the stimulation of red blood cell production.
How you will prepare for the test depends on the problem. You will likely be asked not to eat or drink for several hours before the exam. Your health care provider will go over what you need to do.
How you will prepare for the test depends on the problem. You will likely be asked not to eat or drink for several hours before the exam. Your health care provider will go over what you need to do.
There is little discomfort. The conducting gel may feel a little cold and wet. The sonographer may press the probe against your abdomen.
You will be lying down for the procedure. A clear, water-based conducting gel is applied to the skin over the abdomen. This helps with the transmission of the sound waves. A handheld probe called a transducer is then moved over the abdomen.
An ultrasound machine makes images of organs and structures inside the body. The machine sends out high-frequency sound waves that reflect off body structures. A computer receives these waves and uses them to create a picture. Unlike with x-rays or CT scans, this test does not expose you to ionizing radiation.
The meaning of abnormal results depends on the organ being examined and the type of problem. Talk to your provider if you have any questions or concerns.
Kel Vin Woo, Isabel Y. Shen, Carla J. Weinheimer, Attila Kovacs, Jessica Nigro, Chieh-Yu Lin, Murali Chakinala, Derek E. Byers, David M. Ornitz
You may need to change position so that the health care provider can look at different areas. You may also need to hold your breath for short periods during the exam.
Reviewed by: Jason Levy, MD, FSIR, Northside Radiology Associates, Atlanta, GA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

There is little discomfort. The conducting gel may feel a little cold and wet. The sonographer may press the probe against your abdomen.
Abdominal ultrasound is a type of imaging test. It is used to look at organs in the abdomen, including the liver, gallbladder, spleen, pancreas, and kidneys. The blood vessels that lead to some of these organs, such as the inferior vena cava and aorta, can also be examined with ultrasound.
An ultrasound machine makes images of organs and structures inside the body. The machine sends out high-frequency sound waves that reflect off body structures. A computer receives these waves and uses them to create a picture. Unlike with x-rays or CT scans, this test does not expose you to ionizing radiation. You will be lying down for the procedure. A clear, water-based conducting gel is applied to the skin over the abdomen. This helps with the transmission of the sound waves. A handheld probe called a transducer is then moved over the abdomen.You may need to change position so that the health care provider can look at different areas. You may also need to hold your breath for short periods during the exam.Most of the time, the test takes less than 30 minutes.
Chen L. Abdominal ultrasound imaging: anatomy, physics, instrumentation, and technique. In: Sahani DV, Samir AE, eds. Abdominal Imaging. 2nd ed. Philadelphia, PA: Elsevier; 2017:chap 3.
Barnett CF, Sweeney DA, Huddleston LL. Ultrasonography: advanced applications and procedures. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 24.
The meaning of abnormal results depends on the organ being examined and the type of problem. Talk to your provider if you have any questions or concerns.An abdominal ultrasound can indicate conditions such as:Abdominal aortic aneurysmAbscessAppendicitisCholecystitisGallstonesHydronephrosisKidney stonesPancreatitis (inflammation in pancreas)Spleen enlargement (splenomegaly)Portal hypertensionLiver tumorsObstruction of bile ductsCirrhosis
This is the typical appearance of the blood vessels (vasculature) and urine flow pattern in the kidney. The blood vessels are shown in red and the urine flow pattern in yellow.
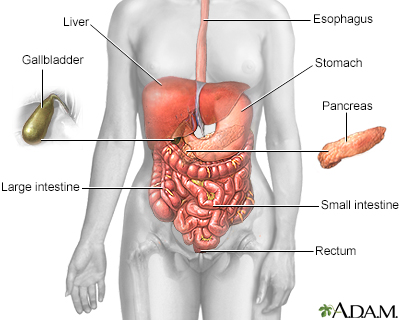
The esophagus, stomach, large and small intestine, aided by the liver, gallbladder and pancreas convert the nutritive components of food into energy and break down the non-nutritive components into waste to be excreted.
The test is done in the ultrasound or radiology department. A conducting paste is applied to your abdomen while you are lying down. The transducer (a hand-held instrument) is then moved over your abdomen.




 Neil
Neil 
 Neil
Neil